Ankle
Injuries
Sprains to the ankle are one of the most common sporting injuries. A sprain is defined as a tearing of the ligaments that connect bone to bone and help stabilise the joint.
Sports requiring jumping, turning and twisting movements such as basketball, volleyball, netball and football; and explosive changes of direction such as soccer, tennis and hockey are particularly vulnerable to ankle sprains.
Following an ankle sprain, the ankle joint may become unstable and take a long time to recover.
Anatomy
The ankle joint is a hinge joint formed between the tibia and fibula (bones of the lower leg) and the talus (a bone of the foot), and allows the foot to bend upwards (dorsiflexion) and downwards (plantarflexion). The joint also allows a small amount of rotation. Two bones of the foot, the talus and calcaneus (heel bone) connect to form the subtalar joint which allows the foot to rock side to side (inversion/eversion).
The joint’s stability comes from the structural arrangement of the bones and the surrounding ligaments. Ligaments provide stability by preventing the amount of side to side movement.
On the inside of the ankle (medial side), the joint is stabilised by a thick, strong fibrous ligament called the deltoid ligament. Sprains to the deltoid ligament (eversion sprains, foot twists outward) account for less than 20% of all ankle sprains.
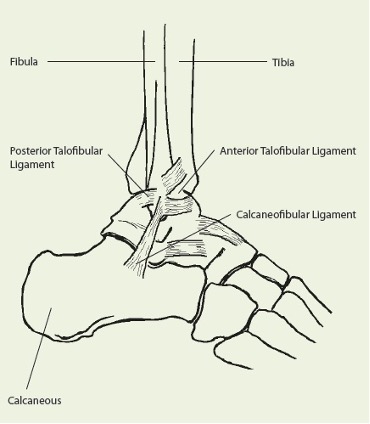
On the outside of the ankle (lateral side), the joint is stabilised by three smaller ligaments; the anterior talofibular (at the front), the calcaneofibular (at the side) and the posterior talofibular (at the back). Sprains to any of these ligaments (inversion sprains, foot twists inward) account for more than 80% of all ankle sprains.
The most commonly injured ligament is the anterior talofibular. Injury to this ligament results in swelling and pain on the outside of the ankle. If the force is more severe, the calcaneofibular ligament is also damaged. The posterior talofibular ligament is less likely to be damaged. A complete tear of all ligaments may result in a dislocation of the ankle joint and an accompanying fracture.
Occasionally medial ligament injuries may be seen in conjunction with a lateral ligament injury.
The inferofebular ligament can also be injured. Injury to this ligament can be a cause of prolonged recovery from a sprain. Ligament sprains to the ankle joint may also involve the ligaments between the tibia and fibula bones. These injuries may involve a fracture, are often slower to recover, and may require surgery.
Risk
Acute ankle sprains result from a force being applied to the ankle joint which causes excessive range of movement at the joint. Players are immediately aware of the condition and may hear an audible ‘snap’ or ‘pop’, due to the tearing or stretching of the ligaments.
Proven risk factors
- Previous or existing ankle injury especially if poorly rehabilitated (biggest risk factor).
- Lack of strength and stability related to the ankle.
- Lack of, or extreme flexibility, in the ankle joint.
- Poor balance.
- Sudden change in direction (acceleration or deceleration).
- Increasing age of player.
Suspected risk factors
- Poor condition of the playing surface.
- Inappropriate, inadequate, or no warm-up.
- Wearing inappropriate footwear for the activity.
- Lack of external ankle support (taping, bracing) for previously injured ankles.
Prevention
- Undertaking training prior to competition to ensure readiness to play.
- Gradually increasing the intensity and duration of training.
- Undertaking flexibility, balance, stretching and strengthening exercises in weekly training programs.
- Including agility work in training programs so the ankle joint is capable of sustaining high acceleration forces and quick changes in direction.
- Allowing adequate recovery time between workouts or training sessions.
- Warming up to ensure surrounding muscles are ready to support the joint during activity.
- Wearing ankle taping or bracing especially for previously injured ankles.
- Wearing shoes appropriate to the sport that provide stability and support.
- Checking the training and playing area to ensure a flat and even surface.
- Drinking water before, during and after play.
- Avoiding activities that cause pain. If pain does occur, discontinuing the activity immediately and commencing RICER.
Signs and Symptoms
Sprains are graded on a scale of 1 to 3 (mild, moderate, and severe), depending on the degree of tearing to the ligaments. In most cases, x-rays are performed to rule out a fracture or dislocation.
| Grade | Description |
| 1 (mild) |
· Minor tear · Minimal pain · Little of no joint instability · Mild pain with weight bearing activities · Slight loss of balance |
| 2 (moderate) |
· Some tearing of the ligament fibres · Moderate to severe pain · Moderate instability of the joint · Swelling and stiffness · Pain with weight bearing activities · Poor balance |
| 3 (severe) |
· Complete tear of the ligament · Severe pain followed by minimal pain · Gross instability of the joint · Severe swelling · Possible pain with weight bearing · Poor balance |
Immediate Management
The immediate treatment of any soft tissue injury consists of the RICER protocol – rest, ice, compression, elevation and referral. RICE protocol should be followed for 48–72 hours. The aim is to reduce the bleeding and damage within the joint. The ankle should be rested in an elevated position with an ice pack applied for 20 minutes every two hours (never apply ice directly to the skin). A correctly sized compression bandage should be applied to limit bleeding and swelling in the joint.
The No HARM protocol should also be applied – no heat, no alcohol, no running or activity, and no massage. This will ensure decreased bleeding and swelling in the injured area.
A sports medicine professional should be seen as soon as possible after the injury to determine the extent of injury and to advise on treatment and rehabilitation. In evaluating the injury, the sports medicine professional may order an x-ray or other testing to determine the extent of the injury.
Rehabilitation and Return to Play
Most ankle sprains heal within 2 to 6 weeks, however severe sprains many take as long as 12 weeks.
A comprehensive rehabilitation program minimises the chance of the injury recurring and includes flexibility, balance, stretching, strengthening and sport specific exercises. During this time, taping or bracing the ankle may be prescribed to provide support until full function is regained. If, while performing a rehabilitation exercise, ankle joint pain or discomfort is experienced, stop immediately and re-consult a sports medicine professional.
Players with significant ligament injuries (Grade 2 or 3) are advised to use bracing or protective taping when playing sport for a minimum of 6 to 12 months post injury.
Acknowledgements
Sports Medicine Australia wishes to thank the sports medicine practitioners and SMA state branches who provided expert feedback in the development of this fact sheet.
Images are courtesy of www.istockphoto.com
Always Consult a Trained Professional
The information above is general in nature and is only intended to provide a summary of the subject matter covered. It is not a substitute for medical advice and you should always consult a trained professional practising in the area of sports medicine in relation to any injury. You use or rely on the information above at your own risk and no party involved in the production of this resource accepts any responsibility for the information contained within it or your use of that information.
