Achilles
Tendon Injuries
Achilles Tendinopathy is a chronic, yet common condition in sports people and recreational athletes. In the past, treatment options have been limited due to a poor understanding of its cause. However, recent research has revealed valuable information that has provided further treatment options.
Until recently, Achilles Tendinopathy was referred to as Achilles Tendinitis. However, research has found that this type of injury does not involve inflammation and is most likely due to a series of micro-tears (tendinosis) that weaken the tendon.
Anatomy
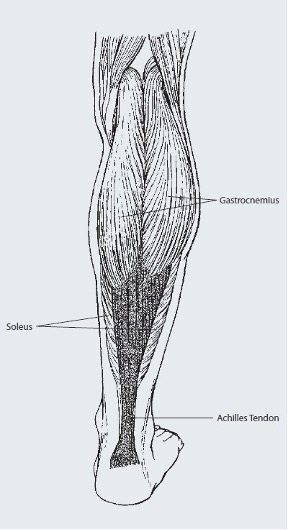
The Achilles tendon is a large tendon at the back of the ankle. The tendon is an extension of the gastrocnemius and soleus (calf muscles), running down the back of the lower leg attaching to the calcaneus (heel bone). The Achilles tendon connects the leg muscles to the foot and gives the ability to push off during walking and running.
Risk
The two most common injuries of the Achilles tendon are Achilles Tendinopathy, and tearing or rupturing of the tendon. Other less common injuries include Peritendinitis and Retrocalcaneal Bursitis. Achilles Tendinopathy can be due to one or a number of causes which may result in excessive loading on the Achilles, including:
- A sudden increase in the intensity, frequency and duration of activity.
- A decrease in recovery time between activity.
- Wearing inadequate or incorrect footwear.
- Excessive pronation (force on Achilles tendon increases).
- Running on hard or uneven surfaces.
- Change of surface (seasonal).
- Poor muscle flexibility (e.g. tight calf muscles, weak calf muscles).
- Decreased joint range of motion (e.g. stiff ankle joint).
- Inadequate warm up, stretching and cool down.
An Achilles tendon rupture is a complete or partial tear that occurs when the tendon is stretched beyond its capacity. Forceful jumping or pivoting, or sudden accelerations of running can overstretch the tendon and cause a tear. An injury to the tendon can also result from falling or tripping. Achilles tendon ruptures are most often seen in ‘weekend warriors’ – typically, middle-aged people participating in sports in their spare time. Less commonly, illness or medications, such as steroids or certain antibiotics, may weaken the tendon and contribute to ruptures.
Prevention
- Wearing appropriate shoes for the activity.
- Using correct technique to limit excessive stress on the Achilles tendon.
- Strapping and taping the ankle to assist in creating a more secure structure.
- Warming up, stretching and cooling down.
- Undertaking training prior to competition to ensure readiness to play.
- Participating in regular strengthening and stretching sessions to maintain muscle strength and flexibility.
- Gradually increasing the intensity and duration of training.
- Allowing adequate recovery time between workouts or training sessions.
- Avoiding activities that cause pain. If pain does occur, discontinuing the activity immediately and commencing RICER.
Signs and Symptoms
Achilles Tendinopathy
- Mild to severe pain and tenderness in the Achilles tendon area (tenderness may be more noticeable in the morning).
- Stiffness that may diminish as the tendon warms up with use.
- Decreased strength and movement – a feeling of sluggishness in the leg.
- Achilles Tendinopathy is graded from 1-4 according to severity.
| Grade | Description |
| 1 (mild) | Pain after running only |
| 2 (moderate) | Pain before and after running; pain gradually lessons during a run. |
| 3 (severe) | Pain with activity causing a decrease in volume of activity. |
| 4 (extreme) | Pain during everyday activities (pain worsening or progressing) |
Achilles tendon injuries
An Achilles tendon can partially tear or completely rupture. While a partial tear presents similar symptoms as a Tendinopathy, a complete rupture causes pain and sudden loss of strength and movement. The pain is likened to a hit or kick in the back of the leg.
Immediate Management
The immediate treatment of any soft tissue injury consists of the RICER protocol – rest, ice, compression, elevation and referral. RICE protocol should be followed for 48–72 hours. The aim is to reduce the bleeding and damage within the joint.
The No HARM protocol should also be applied – no heat, no alcohol, no running or activity, and no massage. This will ensure decreased bleeding and swelling in the injured area.
Treatment includes rest, pain relief, stretching exercises, and changes in sports techniques and footwear to reduce stress on the tendon. Surgery may also be required in some instances.
Rehabilitation and Return to Play
Achilles Tendinopathy that is causing symptoms can require weeks to months of rest for the tendon to slowly repair itself. A sports medicine professional should be seen as soon as possible to determine the extent of the injury and to provide advice on treatment required.
Once pain has settled, a program of rehabilitation exercises may be prescribed to gradually strengthen the tendon to enable it to cope with increased load before return to activity.
The use of crutches may be recommended to keep weight off the injury. Taping, a heel raise or even a plaster cast may also be used if the injury is severe. Other treatments may include ultrasound, mobilisation, stretching, sports massage and orthotics. Anti-inflammatory medication may also be prescribed to reduce pain.
A completely ruptured Achilles tendon is most often repaired surgically. Surgery is often followed by immobilisation in a plaster cast for up to nine weeks. Following this immobilisation period, the Achilles tendon will require intense rehabilitation followed by a strengthening program. These will be completed under the supervision of a sports medicine professional.
Return to activity should be gradual. When returning to activity, a heel raise or taping may be used to reduce the load on the weakened Achilles tendon.
Acknowledgements
Sports Medicine Australia wishes to thank the sports medicine practitioners and SMA state branches who provided expert feedback in the development of this fact sheet.
Images are courtesy of www.istockphoto.com
Always Consult a Trained Professional
The information above is general in nature and is only intended to provide a summary of the subject matter covered. It is not a substitute for medical advice and you should always consult a trained professional practising in the area of sports medicine in relation to any injury. You use or rely on the information above at your own risk and no party involved in the production of this resource accepts any responsibility for the information contained within it or your use of that information.
